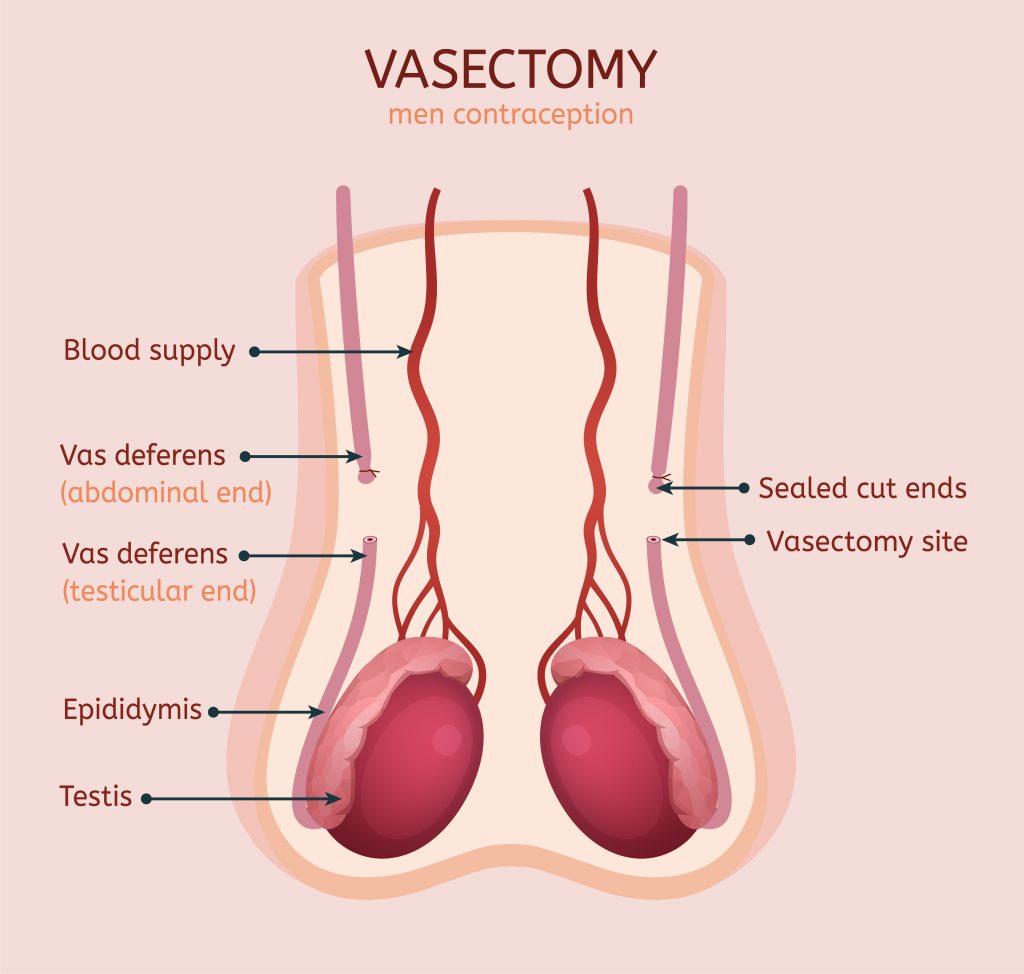
A vasectomy is an operation that makes a man permanently unable to get a woman pregnant.
Sperm are made in the testicles. The sperm from each testicle typically travels through a tube called the vas deferens and mixes with the seminal fluid produced by the seminal vesicles and prostate fluid made by the prostate gland. The sperm, seminal fluid, and prostate fluid make up the semen. During ejaculation (“coming”), the semen goes through the penis and outside the body.
A vasectomy involves cutting the vas deferens on each side so that sperm can no longer get into the semen.

A vasectomy is done in your doctor’s office. The operation takes about half an hour. You’ll be awake during the procedure. Your doctor will give you a local anesthetic to numb your scrotum (the sac of skin that holds your testicles).
After you’re numb, your doctor will make a small opening on one side of your scrotum and pull out part of the vas deferens on that side. You may feel some tugging and pulling. A very small section of the vas deferens is removed. The ends of the vas deferens where the section has been taken will be sealed by stitching them shut, by searing them shut with heat, or by using another method. Your doctor will then do the same thing on the other side.
Your doctor will close the two openings in your scrotum with stitches. After three to 10 days, the stitches will disappear by themselves.
Another type of vasectomy called the no-scalpel vasectomy, involves working through a very small puncture (a hole) in the scrotum. The puncture is so small that it heals without stitches. Once through the skin, the techniques are the same. This type commonly has lower risks for bleeding and infection. The modified no-needle, no-scalpel vasectomy involves using a pressurized jet injector to fire a thin spray of the local anesthetic directly into the tissue, followed by a needle to provide a longer-lasting effect.
Vasectomy may be the safest, most effective kind of birth control. Only about 15 out of 10,000 couples get pregnant the first year after a vasectomy. This is a better result than any other type of birth control besides not having sex.
The use of condoms, barrier devices, oral contraceptive therapy (birth control pills), and tubal ligation are all options for temporary or permanent birth control. You may also consider sperm cryopreservation, which means freezing sperm for use later in life as a backup plan before undergoing a vasectomy. Go to MeetFellow.com and use code Tulane.
Don’t have a vasectomy unless you’re sure you don’t want to have children in the future. Your doctor will probably talk to you to make sure you understand this. Other reasons you may need to wait to have a vasectomy or may not be able to have one include having an infection on or around your genitals or having a bleeding disorder.
Some vasectomies can be undone or “reversed,” but the surgery is expensive and must be performed in a hospital. Even though most men can ejaculate sperm after the reversal surgery, the sperm are often not able to fertilize an egg. The likelihood of pregnancy declines the longer you wait to have the vasectomy reversed. Most men who decide to reverse a vasectomy do so because they get remarried and change their minds about having children.
Before the procedure day, shave the hair off of your scrotum (mainly upper and center areas) and next to the base of the penis with a fresh razor. (Seriously, a razor, not clippers)
On the day of the operation, bring underwear to support the scrotum with you and make sure your genital area is clean (jockstrap, athletic supporter, tight underwear, or compression shorts. There are several types of vasectomy underwear on Amazon.com that come with ice packs).
If you like, you can bring music and headphones to help you relax during the operation.
Right after the operation, your doctor recommends you relax at home for a couple of hours with an ice pack placed on your scrotum. Do not place the ice directly on your scrotal skin to avoid frostbite.
You may have some bruising in the area of the surgery. The bruises should slowly lighten and be gone in about two weeks. You should feel back to normal within a couple of weeks.
Rest with your legs elevated or lie on your back for the first eight hours after the operation. Raise your testicles slightly by putting a rolled-up washcloth under your scrotum. Place an ice pack rolled in another towel on top of your scrotum. Keep your jockstrap on and place the ice pack outside of it.
Keep the area dry for 24 hours.
Take it easy for a couple of days. Use an ice pack when resting.
Avoid strenuous activity, including heavy lifting, for a week.
Wear supportive underwear (jockstrap, athletic supporter, tight underwear, or compression shorts) for the first week or as long as needed to ease the aching feeling.
Avoid having sex or ejaculating for the first week after the operation.
Use another type of birth control until your doctor tells you that your semen is clear of sperm.
Not everyone clears on the first sample, so paying attention to the result is important.
Ask your doctor about stopping blood thinning medications like Coumadin, Warfarin, and Plavix. All of these can thin your blood and cause bleeding. Some patients take medications like Ibuprofen and Tylenol, while some don’t take pain medication at all. Start taking 2 Tylenol Extra Strength pills the morning of the procedure. Try Ibuprofen to relieve pain further. We recommend taking these before using any opioid pain medication because the narcotic (oxycodone, Percocet) may cause nausea, dizziness, confusion, and constipation, and you should not drive while on opioids. We also found that common anti-anxiety meds are not very effective when used for the procedure.
If you have a desk job, expect to return to work after a couple of days. If you do physical labor, walk, or drive a lot, talk to your doctor about when you can return to work.
No. You’ll need to ejaculate at least 15-20 times before the sperm will be cleared from both the vas deferens. For that reason, keep using some form of birth control. Your doctor will ask you to bring in samples of your ejaculation after the operation. Only after you have one sperm-free sample will you be considered unable to get a woman pregnant. This may take three months or longer.
Problems that might occur after your vasectomy include bleeding, infection, and a small lump in the scrotum (a usually mild inflammatory type of reaction to sperm that may have gotten loose during surgery called a sperm granuloma). Call your doctor if you notice any of these signs:
Another risk is that the two ends of the vas deferens may find a way to create a new path to one another. This doesn’t occur very often. But if it does happen, sperm can get into your semen, and you’ll be able to cause a pregnancy.
Vasectomies don’t raise the risk of heart disease. Medical journals report that about 1-2% of men develop significant chronic pain in the scrotal sac after vasectomy. This pain can last for months or years and can even be permanent. This is usually treated with anti-inflammatory drugs. Few men have pain that is severe enough to require additional surgery.
Once sperm can’t get through the vas deferens, your testicles will begin making fewer sperm. Your body will absorb the sperm that are made. But your testicles will keep making testosterone, a male sex hormone, just as they did before the vasectomy.
After you have healed from the vasectomy, your sex life shouldn’t change at all. You will still ejaculate almost the same amount of semen as you did before (sperm is only 2% of the semen), and you won’t notice a change in your sex drive. Some men report having an even stronger sex drive because they no longer have to worry about pregnancy.
Special Notes*
PLEASE EAT and DRINK normally on the day of the procedure.
Increase your fluids the day before your procedure.
Bring a list of your current medications and allergies.
Take your prescribed medications with sips of water the morning of the procedure. If you take Aspirin, Coumadin, or any other blood-thinning medication, please discuss stopping in advance with your doctor. NSAIDS like Ibuprofen, Aleve, Naproxen are ok.
If you have diabetes – take your diabetic medications and check your sugar before arriving.
Bring a jock strap or some supportive undergarment for after the procedure.
Please understand that if you are more than 15 minutes past your arrival procedure time, your appointment might be canceled and must be rescheduled.